
- Key messages
- Cancer in Europe
- Causes of cancer
- Alcohol consumption and cancer risk
- Carcinogenic effects of alcohol
- Alcohol consumption and reduced risk of certain cancers
- Cancer risk after alcohol drinking cessation
- Alcohol consumption before and after breast cancer diagnosis
- Infographic: Beer and Cancer
Key messages
- Most alcohol-related cancers are those of the breast, colorectum, head and neck, liver and oesophagus.
- Substantial numbers of alcohol-related cancers in Europe are associated with consumption of more than 24 g per day for men and more than 12 g per day for women.
- In men, about 3% of alcohol-related cancer cases are associated with consumption of less than 24 g per day. For women only 1% of alcohol-related cases are seen with a consumption of less than 12 g of alcohol per day.
- Alcohol can increase cancer risk even at low levels. With breast cancer for example, consumption of 10 g per day is associated with an increased relative risk of 3–9%. In comparison, using the birth control pill is associated with increased relative risk of 24%.
- All statements on increased and reduced risk must be put into the context of the absolute lifetime risk of getting such cancers.
- There are indications of lower risk for kidney cancer, non-Hodgkin lymphoma and thyroid cancer, associated with moderate alcohol consumption.
Cancer in Europe
More than 3.4 million new cases of cancer were diagnosed in Europe in 2012. 184Cancer is a leading cause of death, comprising around 20% of the total number of deaths each year. 185In 2012, the most common cancer sites were cancers of the female breast (458,337 cases), followed by the colorectum (446,801), lung (409,911) and prostate (399,964). These four cancers represent half of the overall burden of cancer in Europe. The most common causes of death from cancer were cancers of the lung (353,580 deaths), colorectum (214,727), breast (131,259) and stomach (107,313).186
Causes of cancer
The majority of the cancers worldwide are due to exogenous causes. Only a minor part of all cancers are due to endogenous causes such as genetic prediposition. 187Cigarette smoking is the largest preventable cause of cancer in Europe. Other major risk factors for cancer are an unhealthy diet (low intake of fruit and vegetables, high intake of red and processed meats, high calorie intake), and physical inactivity. Alcohol consumption and environmental issues (exposure to the sun, pollutants, infections, etc.) also contribute to cancer risk. 188A substantial part of the cancer cases attributable to alcohol consumption in Europe is associated with a daily alcohol consumption of more than 24 g for men and more than 12 g for women.189
| Table 4. Incidence, mortality, alcohol attribution and cumulative risk, of cancers associated with alcohol consumption in Europe (2012) | ||||||||
|---|---|---|---|---|---|---|---|---|
| Cancer | Incidence.186 | Mortality.186 | Alcohol attributable fraction*180 | Cumulative risk range** | ||||
| Men | Women | Men | Women | Men | Women | Men | Women | |
| Breast (women only) | NA | 458,337 | NA | 131,259 | NA | 5% | NA | 4.2 – 11.6% |
| Colorectal | 241,621 | 205,180 | 113,168 | 101,559 | 17% | 4% | 1.1 – 7.4% | 0.9 – 4.1% |
| Head and neck*** | 109,837 | 29,694 | 52,354 | 11,116 | 0.7 – 4.7% | 0.1 – 0.9% | ||
| Oesophagus | 35,069 | 10,785 | 30,310 | 9,194 | 44% | 25% | 0.1 – 1.2% | 0 – 0.4% |
| Liver and intraheptic bile ducts | 42,783 | 20,637 | 39,899 | 22,253 | 33% | 13% | 0.2 – 1.5% | 0.1 – 0.7% |
NA – not applicable
** The lowest and the highest risk (differs between countries within Europe) of getting a specific cancer up to 75 years old. Data derived from globocan.iarc.fr.
*** Lip, oral cavity, pharynx and larynx
Alcohol consumption and cancer risk
Population studies have shown that consumption of alcoholic beverages may increase the risk of developing cancers of the female breast, colorectum, head and neck, liver and oesophagus.190For cancer prevention it is better not to drink alcohol. 188However, many cancer cases in Europe related to alcohol consumption are associated with daily consumption of more than 24 g of alcohol for men and more than 12 g of alcohol for women.189This also partly explains the higher part of the J-shaped curve between alcohol consumption and all cause mortality. With moderate consumption there is a lower risk for all cause mortality (see Chapter 10).
Alcohol attributable fractions
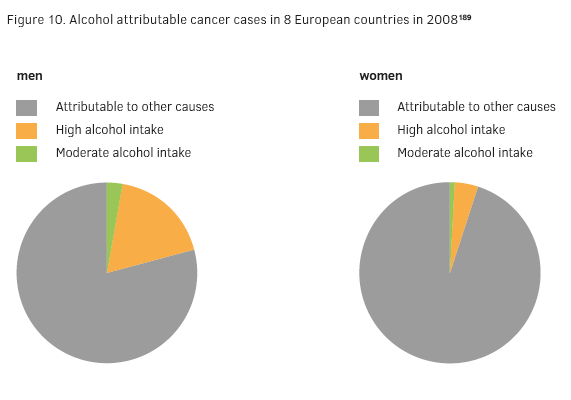
Table 4 gives an overview of the incidence and mortality of alcohol-related cancers in Europe, and the alcohol attributable fractions. This indicates those cases associated with alcohol consumption, or how many cancers could have been prevented if everyone in Europe had always abstained from alcohol. Overall in Europe, cancer cases attributable to alcohol have been estimated to be about 10% of all cases for men and about 3% for women, varying across countries due to differences in intake and other factors. 189A substantial part of alcohol-related cancer cases in Europe are associated with consumption of more than 24 g per day for men and 12 g per day for women. In men, about 3% of alcohol-related cancer cases are associated with consumption of less than 24 g of alcohol per day and more than 18% are associated with consumption of more than 24 g alcohol per day. For women consuming less or more than 12 g alcohol per day, the equivalent figures for alcohol-related cancers are 1% and 4%, respectively (see Figure 10).189
An example of how to interpret the alcohol attributable fraction data in Table 4
The alcohol attributable fraction for breast cancer is 5%. This indicates that of all breast cancer cases in Europe, 5% are associated with alcohol consumption. The incidence of breast cancer in 2012 was 458,337 cases, and so about 23,000 of these are associated with alcohol consumption. In other words, if all women in Europe had abstained from alcohol during their whole life about 23,000 cases of breast cancer could have been prevented in 2012. Other examples are: if all men in Europe did not consume alcohol during their whole life about 41,000 colorectal cancer and 14,000 liver cancer cases could have been prevented in 2012. Keep in mind that most alcohol-related cancer cases are associated with high alcohol consumption.
Breast cancer
Female breast cancer is the most prevalent cancer in Europe. Alcohol consumption is one of the factors increasing breast cancer risk, as well as high body weight, physical inactivity and the use of the birth control pill. Relative breast cancer risk increases by 3–9% (compared to existing risk) for every 10 g of alcohol consumed per day. 191-196The inconsistency of relative risks found across studies might be partially due to differences in the number of subjects with hormone receptor negative and hormone positive tumours. Non-hormonal pathways such as DNA damage are likely to cause receptor negative tumours. Hormone receptor positive tumours contain receptors for the hormones estrogen and/or progesterone. With alcohol consumption, a higher risk for hormone receptor positive tumours has been reported.197-200 The risk effect of alcohol on breast cancer plays a particularly important role in women with a family history of benign mastopathy (diseases of the breast) or other conditions associated with increased breast cancer risk. 194Although there are indications that there is no relationship with body mass index (BMI) or use of hormones, there are still many other aspects that need to be clarified, such as the effects of the age when drinking started, drinking patterns, menopausal status and genetic polymorphisms.201
Colorectal cancer
Colorectal cancer is the second most common cancer in Europe. Red meat consumption, physical inactivity and obesity are risk factors for colorectal cancer, as well as high alcohol consumption. The relative risk of cancers of the colon and rectum appear not to increase with consumption of up to 10 g alcohol per day. 202-204With consumption of 25, 50 and 100 g alcohol per day, the relative risk is increased (compared to existing risk) by 8%, 14% and 43%, respectively, in comparison with non-/occasional drinkers. 204It is suggested that the detrimental effect of drinking on colorectal cancer risk is stronger in men than in women. 202The relative risk for colorectal adenoma, the established pre-cancerous lesion for colorectal cancer, is increased by 27% (compared to existing risk) with each 25 g increment of alcohol intake per day.205
Cancers of the head and neck
For cancers of the head and neck, alcohol consumption is a risk factor, particularly in combination with smoking. In Europe, the highest absolute number of cancer cases attributable to alcohol in men is for upper aerodigestive tract cancers (see Table 4), a substantial part being associated with consumption of more than 24 g of alcohol per day. 189No increase in relative risk for head and neck cancer was found with daily consumption of 12–24 g alcohol, but more than 36 g alcohol per day doubled the relative risk (compared to existing risk) as compared to abstainers. 206Smoking is also a risk factor for cancers of the head and neck, doubling the relative risk with 1–20 cigarettes per day compared to non-smokers. Together, smoking (1–20 cigarettes per day) and high alcohol consumption (more than 36 g per day), have a greater than multiplicative joint effect on the risk of cancers of the head and neck, resulting in a 10 fold increase in relative risk compared to non-drinkers.206
Liver cancer
The incidence and the cumulative risk of liver cancer in Europe is low (see Table 4). Alcohol consumption is a risk factor for liver cancer, and excessive consumption is associated with increased risk. Consumption of 12 g alcohol per day is associated with an increase in the relative risk of liver cancer of 8% (compared to existing risk), and the relative risk is 54% higher with an alcohol consumption of 50 g per day. A separate analysis in people without hepatitis infection indicated that their risk of liver cancer increases when they consume more than 40 g of alcohol per day.207
Oesophageal cancer
The incidence and thus the cumulative risk of oesophageal cancer in Europe is also low (see Table 4). Alcohol consumption is a risk factor for this type of cancer, but the risk is mainly increased with high intake. Alcohol consumption is a risk factor especially for a particular oesophageal cancer called oesophageal squamous cell cancer. Consumption of less than 12.5 g alcohol per day increases the relative risk by 26% (compared to existing risk),202 the relative risk being doubled with alcohol consumption up to 50 g per day, and increased five fold with more than 50 g per day, as compared to non-drinkers.
Carcinogenic effects of alcohol
The possible mechanisms by which alcohol consumption increases the risk of certain cancers are complex and not fully understood.
Acetaldehyde and carcinogenic reactive oxygen species
Acetaldehyde, a toxic metabolite of alcohol, plays a major role in cancer risk.208 At higher consumption levels above 40 g alcohol per day for at least a week, the microsomal ethanol oxidizing system (MEOS) is activated. This alcohol breakdown pathway produces carcinogenic reactive oxygen species (for details of the alcohol metabolism, see Chapter 3). Also bacterial microbiota can metabolise alcohol into acetaldehyde. This is mainly the case with high levels of alcohol in the oral cavity and colorectal areas.209-211
Other possible mechanisms
- Alcohol consumption may also stimulate carcinogenesis by inhibiting DNA methylation and by interacting with retinoid metabolism.208
- Alcohol may alter the metabolism of hormones, such as increasing blood sex hormone levels (e.g. oestrogen), 212,213which may promote the development of breast cancer.
- Alcohol acts as a dissolvent, making it easier for carcinogenic compounds such as those found in cigarettes, to enter tissues.206
- Alcohol-related malabsorption and deficiency of nutrients like folate are associated with different forms of cancer, which can occur with high alcohol consumption.214
Carcinogenic components other than alcohol
Although alcohol is identified as the most important carcinogen in alcoholic beverages, other compounds such as ethyl carbamate and acetaldehyde may also pose risks. 215In the 1980s, beer received much attention due to the discovery of high levels of nitrosamines, 216identified as potential carcinogenic compounds. 217Brewing processes have been optimised since then, and today, there are only negligible amounts of nitrosamines present in beer.218
Alcohol consumption and reduced risk of certain cancers
For certain types of cancers, some risk reduction is seen with alcohol consumption. However, more research is needed to confirm the findings from these population studies and to find the physiological mechanism explaining the effects. 202The cancers are not the most common cancers. Table 5 provides an overview of the incidence and mortality of these specific cancers, and cumulative risk which indicates the risk of getting that type of cancer up to an age of 75 years. The cumulative risk differs between European countries because of differences in risk factors in each. By knowing this risk, it is possible to put relative risks into perspective (see Box at the start of this chapter). If cumulative risk is very small, even a huge decrease in relative risk due to alcohol consumption may not make much absolute difference. But for a cumulative risk that is quite large already, smaller decreases in relative risk can have a big impact.
| Table 5. Incidence, mortality and cumulative risk of the cancers that might be reduced by alcohol consumption in Europe (2012) | ||||||
|---|---|---|---|---|---|---|
| Cancer | Incidence186 | Mortality186 | Cumulative risk range* | |||
| Men | Women | Men | Women | Men | Women | |
| Kidney including renal, pelvis and urethra | 71,739 | 43,435 | 31,313 | 17,678 | 0.44 – 2.91 | 0.22 – 1.22 |
| Non-Hodgkin lymphoma | 49,533 | 43,900 | 20,347 | 17,553 | 0.10 – 1.47 | 0.09 – 1.05 |
| Thyroid | 12,283 | 40,654 | 2,066 | 4,270 | 0.02 – 0.67 | 0.22 – 2.02 |
| Hodgkin’s lymphoma | 9,284 | 8,300 | 2,621 | 2,001 | 0.04 – 0.26 | 0.05 – 0.23 |
* The lowest and the highest risk (differs between countries within Europe) of getting a specific cancer up to age of 75 years old. Data derived from globocan.iarc.fr.
Kidney cancer
The relative risk of kidney cancer decreases (compared to existing risk) by up to 29% with the consumption of up to 50 g of alcohol per day compared to abstainers.202,219,220
Non-Hodgkin lymphoma
Compared with non-drinkers, those consuming alcohol have a 15% lower relative risk (compared to existing risk) for non-Hodgkin lymphoma. The dose-response relationship indicates the relative risk is significantly reduced by 20% with alcohol consumption of up to 75 g per day.223
Thyroid cancer
A significant inverse association is observed between alcohol consumption and thyroid cancer risk. Alcohol consumption of 14–108 g per week decreases the relative risk for thyroid cancer by 17% (compared to existing risk), and consumption of more than 108 g alcohol per week decreases the relative risk by 28% as compared to abstainers. 221Similar findings are observed in a follow-up study where alcohol consumption of 15 g per day or more was associated with a 23% lower relative risk of thyroid cancer compared with those consuming 0.1–4.9 g alcohol per day.222
Hodgkin’s lymphoma
Hodgkin’s lymphoma is a rare cancer in Europe, as also indicated by the low cumulative risks. Compared with non-drinkers, those consuming alcohol have a 30% lower relative risk (compared to existing risk) for Hodgkin’s lymphoma. An inverse dose-response relationship has also been indicated, but as it was not significant, caution is required in the interpretation of findings.224
Cancer risk after alcohol drinking cessation
It is difficult to estimate how long it takes for such elevated risks to decrease or disappear after someone stops drinking alcoholic beverages. Research is limited and not unequivocal. For mouth and throat cancer it may take more than 35 years to disappear225 and for oesophageal cancer and liver cancer, 16.5 and 23 years, respectively.226,227
Alcohol consumption before and after breast cancer diagnosis
Alcohol consumption before and after breast cancer treatment, appears to have limited effects on survival.
Before diagnosis and survival
Based on a large population study of women with breast cancer, there was some indication that consumption of 42–84 g per week modestly improved breast cancer survival by 15% (relative risk) as compared to non-consumers and those who consume more.228
After diagnosis and survival
Alcohol consumption of more than 140 g per week after breast cancer diagnosis is associated with a reduced relative risk of death from cardiovascular disease (CVD) of 53% and a reduced relative risk of overall mortality of 36% 228 CVD is an important contributor to mortality among breast cancer survivors, probably because of the cardiotoxic and metabolic effects of some breast cancer treatments.229
What is cancer?
Cancer is a collective term for more than 100 different diseases which are all characterised by uncontrollable and abnormal cell growth. This growth is caused by a change in the DNA that controls cell division, and tumours form when abnormal cell growth occurs over a long period of time. Malignant tumours can invade other tissues and spread in the blood and lymphatic system causing metastasis (occurrence of tumours in other parts of the body). Benign tumours do not spread, and eventually stop growing. Only malignant tumours are called cancer.230
Relative risk tells you nothing about absolute risk
In this chapter you can read about alcohol consumption increasing or lowering the risk of certain types of cancer. It is important to realise that these figures present relative risks. They tell us how much more or less likely the cancer occurs in a group consuming alcohol compared to others not consuming alcohol. This is different from the overall likelihood of getting cancer in your life, i.e. the absolute lifetime risk. The cumulative risk in Table 4 indicates the absolute risk of getting certain types of cancer up to an age of 75 years old. This risk differs between European countries, depending on particular risk factors in each. By knowing the cumulative risks, it is possible to place the relative risks mentioned in this chapter into perspective, as shown in the example below and the breast cancer example included later. If the cumulative risk is very small, even a huge increase in relative risk due to alcohol consumption may not make much absolute difference. But for a cumulative risk that is quite large already, smaller increases in relative risk can have a large impact.
Example:
The highest absolute lifetime risk for European men up to 75 years old contracting colorectal cancer is 7.4% (see Table 4), which occurs in Slovakia. Consumption of 25 g of alcohol per day increases the (relative) risk by 8% (Section 7.3), equivalent to an increase, due to alcohol consumption in absolute risk from 7.4% to 8.0%, or an increase from 74 to 80 of 1,000 men who develop colorectal cancer.
However keep in mind these are just examples that give an impression of the effect of alcohol consumption on the absolute lifetime risk up to an age of 75 years old. Individual absolute lifetime risk may be higher or lower than these figures depending on particular risk factors such as age and lifestyle.
Remember: Each glass of an alcoholic beverage increases the risk of breast cancer
There are multiple risk factors for breast cancer, and alcohol consumption is one of them. The highest lifetime risk of developing breast cancer in Europe up to an age of 75 years old (see Table 4) is 11.6%, as reported from Belgium. Each glass of alcoholic beverage per day (10 g of alcohol) increases the risk by 3–9%, 191meaning the absolute risk increases from 11.6% to 12.0–12.6% (a 0.4–1.0 percentage point increase). This corresponds to an increase from 116 to 120–126 women out of 1,000 who develop breast cancer. To put this in perspective, another risk factor for breast cancer is the birth control pill, and using this pill increases the risk by 24% 231increasing absolute risk from 11.6% to 14.4% (an increase from 116 to 144 women out of 1,000 who develop breast cancer). Keep in mind these are just examples that indicate the effects of alcohol consumption and using the birth control pill on the absolute lifetime risk of developing breast cancer up to an age of 75 years old. Absolute lifetime risk may be higher or lower than these figures depending on particular risk factors such as age and lifestyle.
This is not intended to discourage use of the birth control pill but rather to put into some context the impact of alcohol consumption.







