A large study1 published in The Lancet investigates cancer burden attributable to potentially modifiable risk factors. The researchers found that worldwide 44.4% of cancer deaths and 42% of DALY’s (=disability-adjusted life-years) are attributable to modifiable risk factors like smoking, unhealthy diet, drinking alcohol and high BMI.
What is already known? Cigarette smoking is the largest preventable cause of cancer in Europe. Other major risk factors for cancer are an unhealthy diet (low intake of fruit and vegetables, high intake of red and processed meats, high calorie intake), and physical inactivity. Alcohol consumption and environmental issues (exposure to the sun, pollutants, infections, etc.) also contribute to cancer risk.2
What does this study add? The Global Burden of Diseases, Injuries, and Risk Factors Study (GBD)1 quantifies cancer burden attributable to a broad set of modifiable risk factors worldwide and over time, using both mortality and disability-adjusted life-years (DALYs).
Cancer burden
The GBD 2019 comparative risk assessment framework was used to estimate cancer burden attributable to behavioural, environmental and occupational, and metabolic risk factors. A total of 82 risk–outcome pairs were included on the basis of the World Cancer Research Fund criteria. Estimated cancer deaths and disability-adjusted life-years (DALYs) in 2019 and change in these measures between 2010 and 2019 are presented. In an earlier report, researchers estimated mortality from 12 types of cancer attributable to nine risk factors in seven World Bank regions for 2001.3
Leading risk factor is tobacco
The leading risk factors globally for risk-attributable cancer DALYs in 2019 for both sexes combined were tobacco (23.7%), followed by dietary risks (5.6%), alcohol use (5.2%) and high BMI (4.5%).
Ranking of risk factors by attributable cancer deaths globally in 2019 showed similar ranking as by attributable cancer DALYs.
Differences sexes
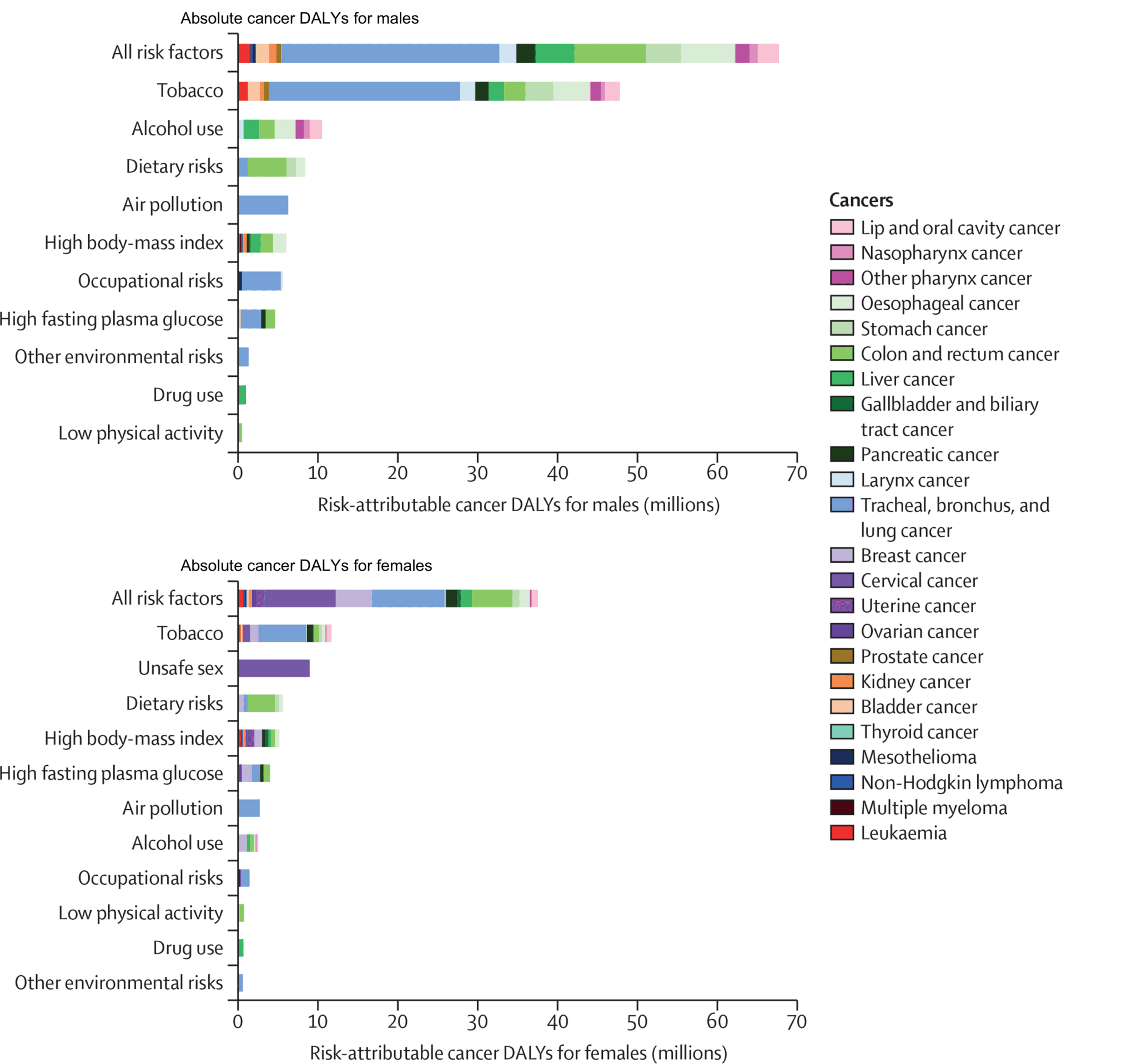
The leading risk factor in males in terms of attributable cancer DALYs is tobacco, which accounts for 33.9% of all cancer DALYs in males in 2019. Alcohol use, dietary risks, and air pollution were the next greatest risk factors, accounting for 7.4%, 5.9%, and 4.4%, respectively, of all male cancer DALYs in 2019.
Tobacco was also the leading risk factor for females globally in terms of attributable cancer DALYs and accounted for 10.7% of all female cancer DALYs in 2019. Unsafe sex was the second leading risk factor for females, accounting for 8.2% of all female cancer DALYs in 2019, followed by dietary risks (5.1%), high BMI (4.7%), and high fasting plasma glucose (3.6%). Alcohol use was risk factor number 8 in females, accounting for 2.3% of all female DALYs in 2019. (See figure 1).
Figure 1: Absolute cancer DALYs for males and females
Early diagnosis and effective treatment
These findings highlight that a substantial proportion of cancer burden globally has potential for prevention through interventions aimed at reducing exposure to known cancer risk factors. But also that a large proportion of cancer burden might not be avoidable through control of the risk factors currently estimated. Thus, cancer risk reduction efforts must be coupled with comprehensive cancer control strategies that include efforts to support early diagnosis and effective treatment.
Strengths
- Large amounts of data used for different risk outcomes for men and women
- Both cancer death and disability-adjusted life-years (DALY’s) taken into account
Limitations
- No distinction in amount or pattern of alcohol consumption
- Based on theoretical model
References
- The global burden of cancer attributable to risk factors, 2010–19: a systematic analysis for the Global Burden of Disease Study 2019. Lancet 400 (2022) 10352, 563-591.DOI: https://doi.org/10.1016/S0140-6736(22)01438-6
- Schüz J, Espina C, Villain P et al. (2015). European Code against Cancer 4th edition: 12 ways to reduce your cancer risk. Cancer Epidemiol, Epub.
- Danaei G, Vander Hoorn S, Lopez AD, Murray CJ, Ezzati M, Causes of cancer in the world: comparative risk assessment of nine behavioural and environmental risk factors. Lancet. 2005; 366: 1784-1793

